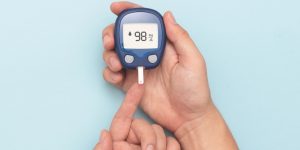
It’s a familiar scenario for many of us. You prick your finger, obtain that tiny blood sample (which always seems disproportionately large), insert it into the meter, and the result appears: a number that seems more suited to a financial report than a glucose reading. The first time this happened to me, my heart raced. I’d indulged in a generous slice of my Aunt Carol’s pecan pie (it truly is a masterpiece!), and my blood sugar had clearly responded.
So, what is the absolute first step you should take after encountering a high blood sugar reading?
Step 1: Take a Deep Breath (Seriously!) and… Retest?
Before considering drastic measures, take a deep, calming breath. Inhale, exhale. Panic often exacerbates the situation. My grandmother, who has managed type 2 diabetes for decades, often says, “Stress elevates blood sugar.” And she’s correct.
Now, here’s a crucial point I learned through experience: glucose meters can occasionally be inaccurate. Perhaps your hands weren’t completely clean (it happens!), or the test strip was compromised. Before taking any further action, retest. Wash your hands thoroughly with soap and water – ensure they are meticulously clean – dry them completely, and use a fresh test strip.
Wait, no—hold on! Ensure your meter itself is functioning properly. Some meters have upper limits to their readings. If the initial number was exceptionally high, consult your meter’s manual to confirm its capabilities.
This second reading is your foundation. It’s the basis for your subsequent actions. Consider it a second opinion, but from a less biased source.
Okay, Now What? (Assuming No ER Trip is Needed)

Let’s assume the second reading remains elevated, but you’re not experiencing any severe symptoms. No nausea, no intense abdominal pain, no rapid breathing (unless you’ve just completed strenuous exercise, in which case, elevated blood sugar might be a secondary concern!). Here’s the immediate action plan:
- Hydrate Extensively (It’s Crucial): Water is essential. Avoid sugary beverages, including diet sodas. Focus on pure, unadulterated water. This helps your kidneys flush out excess sugar. Think of it as assisting your body’s natural filtration system. Avoid caffeine and alcohol, as these can interfere with blood sugar control or lead to dehydration.
- Gentle Movement (Unless Contraindicated by Your Doctor): I’m not suggesting intense exercise. A leisurely walk can be remarkably effective. It signals your muscles to utilize the excess glucose. However – and this is critical – if your blood sugar is exceptionally high (e.g., over 240 mg/dL) and you have ketones (detectable with urine test strips), avoid exercise. Contact your healthcare provider immediately. Exercise in the presence of high ketones can be counterproductive. I learned this the hard way, attempting to “walk it off” and ending up feeling significantly worse.
- Ketone Check!: If your blood sugar is high, use a urine ketone test strip. These are readily available and provide crucial information. The presence of moderate or large ketones is a significant warning sign. Contact your doctor immediately, without hesitation.
- Medication Review (Did You Miss a Dose?): If you’re prescribed insulin or other diabetes medications, reflect. Did you miss a dose? Was the dosage incorrect? If a dose was missed and it’s close to your usual administration time, taking it might be appropriate. However – and this cannot be overemphasized – if you’re uncertain, contact your doctor or a diabetes educator. Medication adjustments require professional guidance.
Beyond the Immediate: Building a Sustainable Blood Sugar Strategy

Those are the immediate, reactive steps. However, a single elevated reading (or even several) is not catastrophic. It’s an indicator. It’s your body communicating, “Attention is required!”
Long-term management is a more complex process, involving factors you’re likely aware of (but may not consistently prioritize):
- Dietary Considerations: Yes, the often-repeated advice: reduce sugar and processed carbohydrates, increase vegetables, and so on. It’s fundamentally true! Approach it as an exploration of healthy, enjoyable options. My personal favorite? Sweet potatoes. Roasted with a touch of cinnamon, they’re a satisfying treat. The “Diabetes Plate method” is also incredibly helpful: visualize your plate divided into sections – half non-starchy vegetables (like broccoli, spinach, or peppers), one-quarter lean protein (such as chicken, fish, or tofu), and one-quarter quality carbohydrates (like brown rice or quinoa).
- Regular Physical Activity: Find an activity you genuinely enjoy. Dancing, hiking, playing with pets – all contribute. The objective is to elevate your heart rate, even briefly. Those short bursts of activity, often called “exercise snacks,” are remarkably effective.
- Medication Adherence: If you’re prescribed medication, take it precisely as directed. Your doctor has carefully tailored your regimen to your individual needs.
- Regular Monitoring (Blood Sugar and Doctor Visits): Consistent blood sugar monitoring is your most valuable tool. It reveals how your body responds to various factors. Regular check-ups with your healthcare team are equally essential. They can identify potential issues early and adjust your plan accordingly.
Emergency Room Red Flags (Do Not Ignore These!)

It’s crucial to reiterate the warning signs. If you have a high blood sugar reading and any of the following symptoms, call 911 (or your local emergency number) immediately:
- Persistent nausea or vomiting.
- Severe abdominal pain.
- Rapid and deep breathing.
- Significant dehydration – headache, dry skin, rapid heartbeat, difficulty staying awake.
- Fruity-smelling breath.
- Confusion or loss of consciousness.
- Blood sugar that remains extremely high (e.g., above 350 or even 600, depending on your doctor’s instructions), despite attempts to lower it.
- Diarrhea or vomiting that prevents the intake of food or liquids.
These could indicate diabetic ketoacidosis (DKA) or hyperosmolar hyperglycemic state (HHS), both of which are life-threatening and require immediate medical intervention.
Understanding Your Blood Sugar Numbers (and Their Significance)
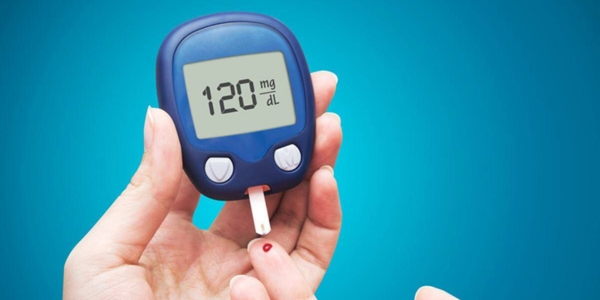
Your doctor should have provided personalized target blood sugar ranges. However, general guidelines suggest:
- Before meals: 80-130 mg/dL
- Two hours after a meal: Less than 180 mg/dL
But remember, these are just guidelines. Your personal targets might be different.
The Bottom Line
A high blood sugar reading can be unsettling, but it’s not a cause for panic. Take a deep breath, retest, and take appropriate action. Remember, you’re not alone. Many individuals are navigating this journey, one blood sugar reading at a time. Open communication with your doctor, dietitian, and diabetes educator is key to achieving and maintaining optimal blood sugar control and preventing complications. And don’t hesitate to ask questions – that’s what your healthcare team is there for! I, for one, had to ask my doctor multiple times about the correct operation of my meter. There’s no shame in seeking clarity.